Introduction
In healthcare, trust is the foundation of the effective patient–provider relationship. Without it, patients may hesitate to follow advice, delay interventions, or avoid care altogether. One powerful—but often underleveraged—strategy to cultivate trust is patient education, and this article explores how patient education builds trust in healthcare by giving patients accessible, clear information about their conditions, treatments, and wellness.
This article explores why patient education matters, how it builds trust, best practices, challenges, and how clinics can integrate it into their digital presence.
1. Why Trust Matters in Healthcare
1.1 The Consequences of Low Trust
Low patient trust has serious implications:
- Poor adherence to treatment or medications
- Increased patient anxiety, confusion, or dissatisfaction
- Higher rates of second opinions or switching doctors
- Lower engagement in preventive care
- Negative word-of-mouth or reputation damage
Especially during times of crisis (e.g. pandemics, vaccine campaigns), mistrust can lead to avoidant behavior or belief in misinformation.
1.2 Dimensions of Trust
In healthcare contexts, trust typically involves:
- Competence: belief that the provider knows what they’re doing
- Benevolence / Intent: belief that the provider acts in the patient’s interest
- Reliability / Consistency: that the provider is dependable over time
- Transparency / Honesty: openness about risks, alternatives, uncertainties
- Communication & Empathy: that the provider listens and respects the patient
Patient education directly contributes toward several of these dimensions, especially competence, transparency, and communication.

2. The Link Between Knowledge and How Patient Education Builds Trust in Healthcare
2.1 Theoretical Foundations
A recent theoretical discussion argues that patients’ knowledge and trust in healthcare personnel are positively related because both are oriented toward future decisions. In uncertain high-modernity societies (where medicine is complex), knowledge helps patients reduce uncertainty—and trust is a mechanism to deal with complexity and risk.
Thus, when patients are better informed about their condition, treatment options, risks, and the reasoning behind decisions, their need to rely on blind faith is reduced. This contributes to more secure and reasoned trust.
2.2 Empirical Evidence
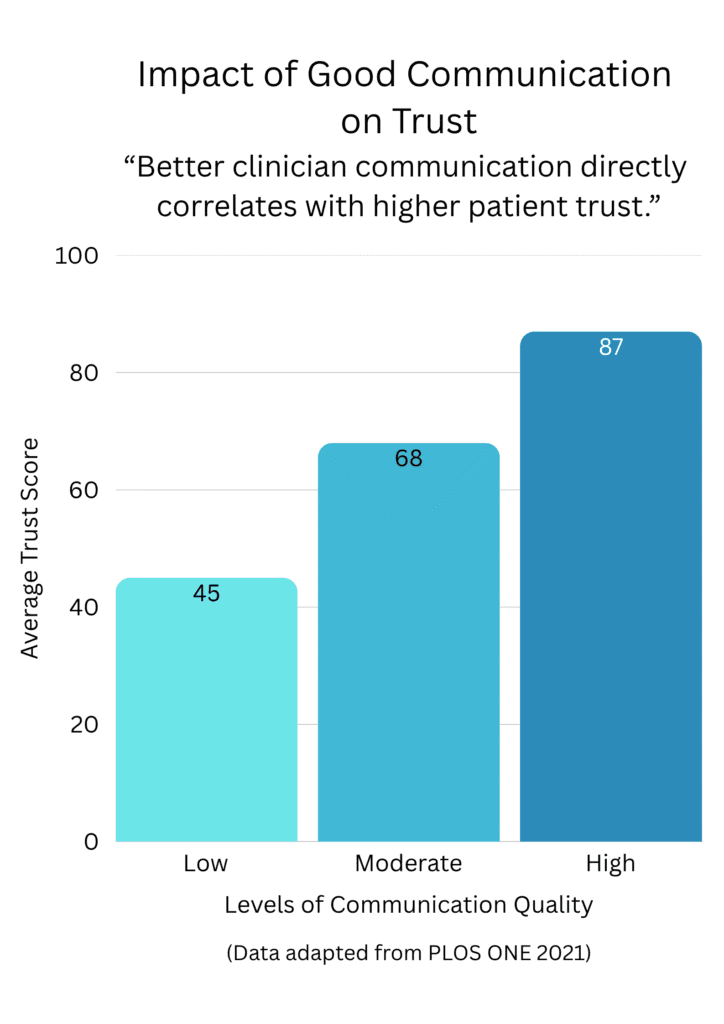
- Clinician communication and trust: A PLOS ONE study analyzed how patient perceptions of clinician communication influence their trust in clinicians as information sources. It found that better patient-centered communication correlates with higher trust.
- Patient portals & education: A systematic review of educational resources via patient portals showed that when patients access well-designed educational content, they show improved knowledge, activation, better self-management, and lower anxiety.
- Student-led education and trust: A study on the impact of patient education sessions (led by medical students) found measurable increases in patient trust in those educational encounters.
- Shared decision-making and trust: Interventions that promote shared decision-making (which often include educational components) show improved patient trust, because patients feel more involved and informed.
These studies support that more informed patients are more trusting patients—but only if the education is thoughtfully delivered.
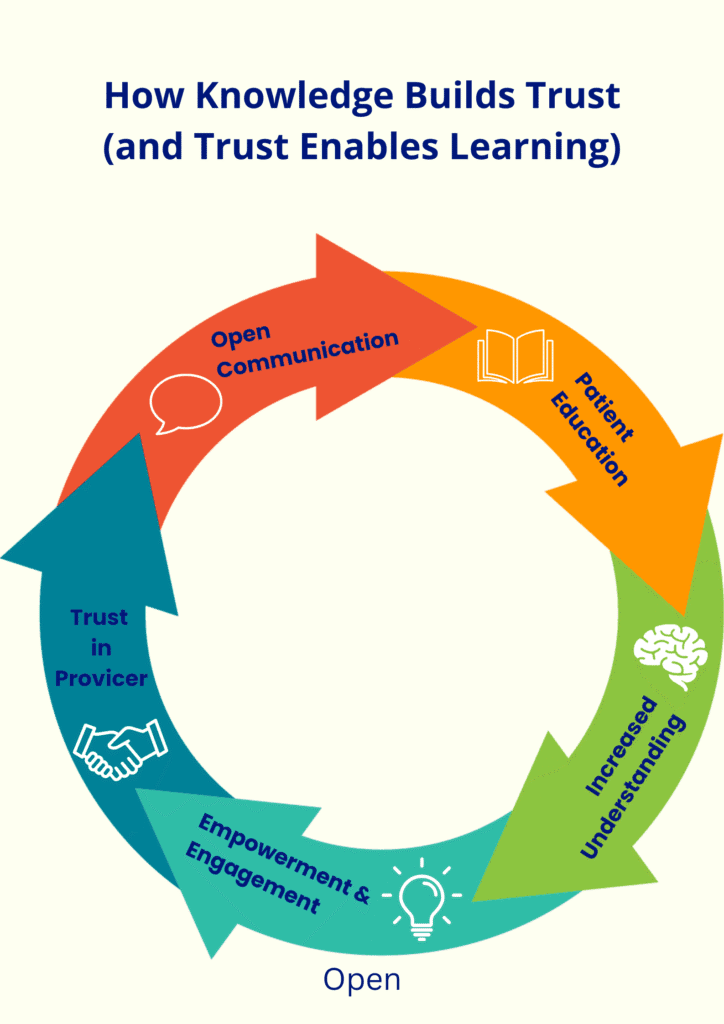
3. How Patient Education Builds Trust: Mechanisms & Effects
Below are key mechanisms by which patient education fosters trust, along with effects clinics can aim for.

3.1 Mechanism: Reducing Information Asymmetry
Healthcare is inherently technical. Patients often lack background in medicine, so providers hold most of the knowledge. This asymmetry can breed suspicion. But education bridges that gap:
- When providers explain in plain terms what’s happening, why a test or treatment is needed, and what risks are involved, patients see competence and transparency.
- This helps demystify decisions—and patients feel less manipulated or “in the dark.”
3.2 Mechanism: Empowerment & Autonomy
Educated patients feel more in control:
- They can ask informed questions.
- They engage more actively in shared decision-making.
- They feel not like passive recipients, but partners.
When a clinic enables that, it signals respect and benevolence—thus building trust.
3.3 Mechanism: Expectation Management & Realistic Framing
Often, unmet expectations breed mistrust (“Why didn’t they tell me this side effect might occur?”). Education helps:
- Setting realistic expectations (benefits, limitations, trade-offs)
- Explaining uncertainties and what is unknown
- Preparing patients for possible outcomes or variations
When surprises are minimized and patients are forewarned, trust is preserved even when things don’t go perfectly.
Often, unmet expectations breed mistrust (“Why didn’t they tell me this side effect might occur?”). Education helps:
- Setting realistic expectations (benefits, limitations, trade-offs)
- Explaining uncertainties and what is unknown
- Preparing patients for possible outcomes or variations
When surprises are minimized and patients are forewarned, trust is preserved even when things don’t go perfectly.
3.4 Mechanism: Consistency Over Time
Trust isn’t built in one session. Educational continuity—through follow-up materials, reminders, FAQs, and consistent messaging—reinforces reliability. If a clinic posts regular, credible educational content online, patients see a pattern: this provider consistently cares about knowledge and transparency.
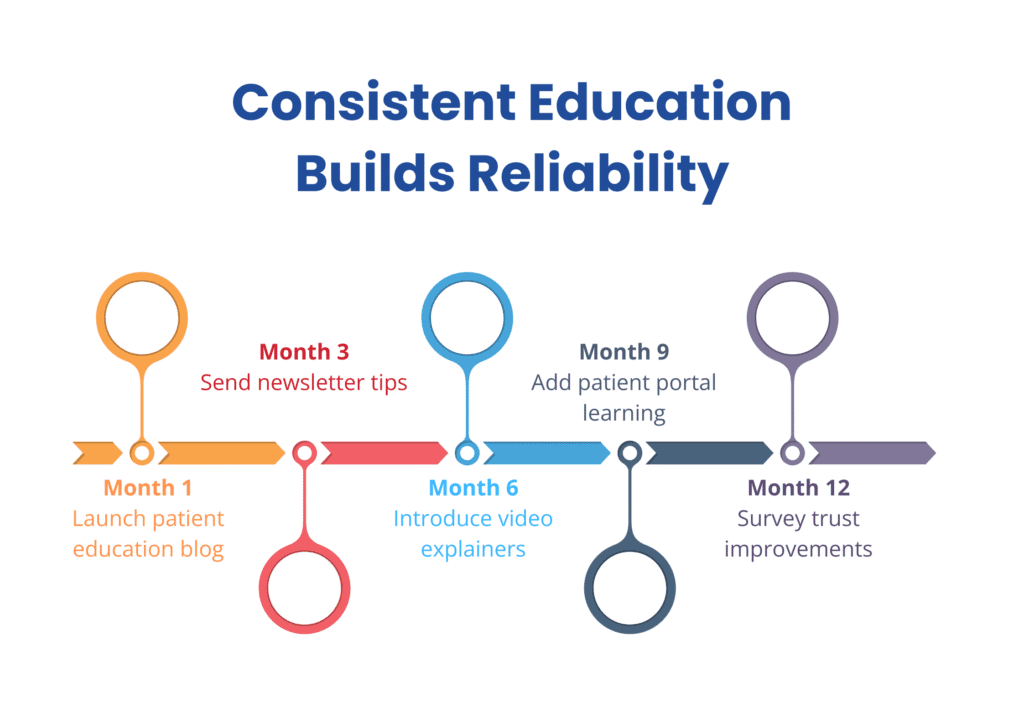
3.5 Mechanism: Feedback Loops & Participation
Effective education isn’t one-way. Incorporating feedback mechanisms—quizzes, “teach-back,” Q&A, forums—lets patients express misunderstandings and get clarifications. When they perceive responsiveness, trust strengthens.
The teach-back method is an example: after explaining, the provider asks the patient to repeat back in their own words. Misunderstandings are caught early, promoting clarity and rapport.
4. Best Practices: How Patient Education Builds Trust in Healthcare for Clinics
To maximize trust through patient education, clinics and presence-management teams (like Tatak Mo) should follow best practices:
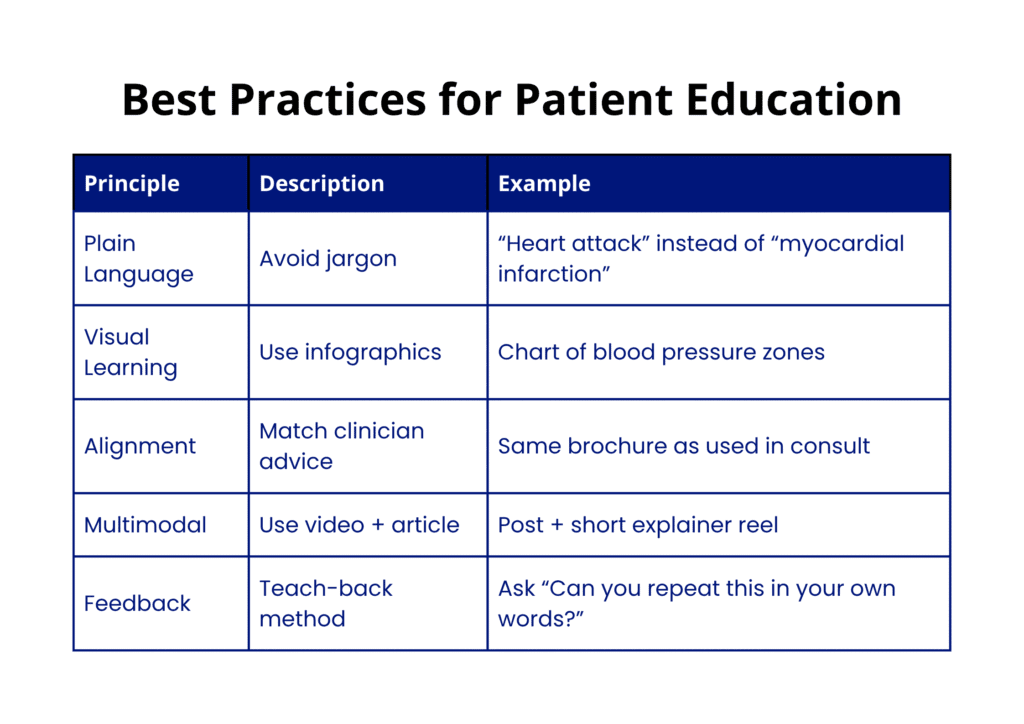
4.1 Design for Readability & Health Literacy
- Use plain language, avoid medical jargon
- Use short sentences, bulleted lists, visuals, infographics
- Provide glossaries or simplified definitions
- Use NLP / AI simplification tools where appropriate to translate jargon to lay terms. (Recent research explores models that convert medical jargon to lay language to improve comprehension)
4.2 Align Education with Clinical Decisions
Patients trust more when educational materials mirror what their doctor is using:
- Use the same evidence sources (guidelines, references)
- Integrate patient education into clinic EHRs or decision support
- Involve clinicians in drafting or approving education content
Wolters Kluwer notes that when materials are aligned with clinical decision-making, it reinforces the perception that the provider and the content are unified and trustworthy.
4.3 Use Multiple Modalities
Different patients absorb content differently:
- Written articles / blog posts
- Infographics
- Short explainer videos
- Interactive modules / quizzes
- FAQ pages
- Webinars / live Q&A sessions
Modality variety helps reach more people and reinforces trust through repeated exposure.
4.4 Leverage Patient Portals & Apps
Integrate education directly where patients engage:
- Push relevant articles in portal dashboards
- Link explanations to lab results, medication instructions, or follow-up plans
- Use contextual pop-up help or “learn more” links
The effectiveness of patient portal–based education is documented: users often increase knowledge, activation, and better outcomes.
4.5 Encourage Shared Decision-Making
Provide decision aids—tools that present options, benefits, harms, and probabilities clearly to patients. These help patients understand trade-offs and participate in decisions.
When patients feel they helped shape the plan, they trust the outcome more—even if it’s suboptimal.
4.6 Monitor & Update Content Regularly
- Review for accuracy (medical guidelines change)
- Use analytics: which articles are read most, where users drop off
- Solicit patient feedback or “What else do you want to know?” prompts
- Address misinformation proactively (especially in social media or blog comments)
- Use exposure to misinformation as education: e.g., “Why this common myth is wrong”
4.7 Cultural & Contextual Sensitivity
- Localize examples (Philippines context, terminologies, disease prevalence)
- Use languages appropriate to the patient audience
- Respect cultural beliefs and tailor messaging that doesn’t alienate
Trust is fragile especially when communications feel foreign or irrelevant.
5. Challenges, Pitfalls & Mitigation
Even well-intended education efforts face hurdles. Here are common challenges and how to address them:
| Challenge | Risk to Trust | Mitigation Strategy |
|---|---|---|
| Information overload / complexity | Patients may feel overwhelmed, lost, or suspicious | Use progressive disclosure (layered content), chunk into digestible pieces |
| Inconsistent messaging vs. provider behavior | Contradictions can erode credibility | Maintain alignment: clinician review, version control, audit content |
| Low engagement or reach | If few patients see or use educational content, it appears tokenistic | Promote via email, social media, in-clinic displays; integrate into care pathways |
| Outdated or inaccurate content | Misinformation backfires | Set regular review cycles; cite sources; date-stamp content |
| Mistrust in digital channels (patients skeptical of “online” content) | Patients ignore or disbelieve the material | Use references, endorsements, third-party validation; blend with face-to-face education |
| Health literacy gaps | Some patients may not understand even “simple” content | Use universal design principles (visuals, analogies, multiple formats), and use teach-back / feedback loops |
6. Real-World Examples & Case Studies
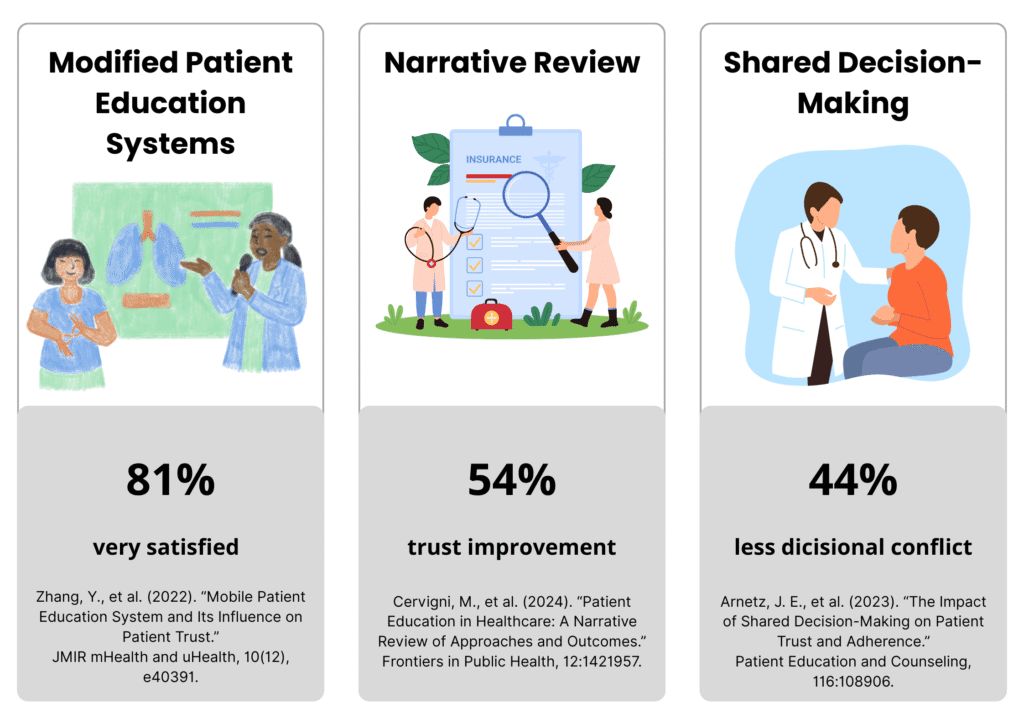
6.1 Mobile Patient Education Systems & Trust
One empirical investigation studied a Mobile Patient Education System (MPES) and its influence on patient trust. The authors found that when patients had access to curated, consistent educational content via the app, their trust in providers increased.
6.2 Narrative Review on Patient Education Approaches
A recent narrative review summarized various approaches (e.g. e-learning modules, printed materials, digital tools) and their relationship to health literacy, empowerment, and trust. It argued that education integrated thoughtfully into clinical workflows strengthens relational trust.
6.3 Shared Decision-Making Interventions
Recent studies show that interventions to increase shared decision-making (which inherently include education of options) result in higher trust scores, particularly when communication improves.
7. A Framework for Clinic Implementation (Step-by-Step)
Here’s a recommended roadmap for clinics (or your Tatak Mo clients) to embed patient education that builds trust:
1. Audit current educational resources
- Inventory blog pages, handouts, portal articles
- Identify gaps, outdated content, conflicting messages
2. Engage clinicians & stakeholders
- Involve doctors, nurses in drafting / approving content
- Align with clinical guidelines and care protocols
3. Define target topics & content plan
- Common conditions in your area
- Preventive care, chronic disease management, wellness
- Misinformation correction
4. Design with trust in mind
- Plain language, visuals, consistent voice
- Use disclaimers, citations, links to scientific sources
- Update dates clearly visible
5. Choose delivery channels
- Clinic website / blog
- Social media (carousel posts, reels, short tips)
- Patient portal / mobile app
- Physical handouts or QR codes linking to digital content
6. Implement feedback & interactivity
- Include quizzes, surveys, “ask us anything” forms
- Use teach-back in clinic visits
- Respond to comments or questions online
7. Promote & integrate
- In structural touchpoints (registration, discharge packets)
- Email newsletters, SMS links
- Signage, staff reminders
8. Monitor & iterate
- Analytics on views, time spent, drop-offs
- Patient surveys: “Was this useful? What else do you need?”
- Regular content review (e.g. quarterly)
9. Evaluate impact on trust & outcomes
- Patient trust surveys (before and after)
- Metrics like revisits, adherence, satisfaction
- Qualitative feedback

By following this framework, a clinic can transform education from a “nice-to-have” to a strategic trust-builder.
8. SEO Considerations & Keywords
To help this article (or variants) rank in search engines, consider optimizing for keywords such as:
- “patient education in healthcare”
- “how patient education builds trust”
- “clinic trust building strategies”
- “healthcare patient information trust”
- “patient education best practices”
Also include internal links (if this is part of a blog site) to related content, and external citations like the ones above to improve credibility.
9. Conclusion
Patient education is not just a supplemental tool—it’s a cornerstone of trust-building in modern healthcare. When done well, it addresses the information gap, empowers patients, aligns expectations, and creates a more transparent and reliable relationship. For clinics and healthcare brands, integrating patient education into your digital presence and care processes can be a powerful differentiator in earning and sustaining patient trust drop by drop.
See how your clinic appears to patients online — and start building digital trust today.
Book Your Free Online Presence Health Check
Your clinic’s online presence shapes how patients perceive your care.
Let’s review your website, social media, and digital visibility —
and identify how you can build stronger patient trust before year-end.
References:
- Trust in Healthcare, Medical Mistrust, and Health Outcomes in Times of Health Crisis: A Narrative Review by Elisavet Souvatzi, Magdalini Katsikidou, Aikaterini Arvaniti, Spyridon Plakias, Anna Tsiakiri, and Maria Samakouri
- Patient Knowledge and Trust in Health Care. A Theoretical Discussion on the Relationship Between Patients’ Knowledge and Their Trust in Health Care Personnel in High Modernity by Stein Conradsen, Henrik Vardinghus-Nielsen & Helge Skirbekk
- How clinician-patient communication affects trust in health information sources: Temporal trends from a national cross-sectional survey by Onur Asan, Zhongyuan Yu, and Bradley H. Crotty
- A systematic review of the effectiveness of patient education through patient portals Open Access by Adam M Johnson, Andrew S Brimhall, Erica T Johnson, Jennifer Hodgson, Katharine Didericksen, Joseph Pye, G J Corey Harmon, and Kerry B Sewell
- Impact of Patient Education on Establishing Trust as the Medical Student Provider: A Student Run Free Clinic Experience by David Salchert, MD1,2; Marley Lee, MD1,2; Chandler Hinson, MBA, MSc1,2; Richard A Perkins, MS1,2; Stephanie Rudolf, DNP, RN1,3
- Can shared decision-making interventions increase trust/trustworthiness in the physician-patient encounter? A scoping review Natalie Strokes, Caroline Lloyd, Abigail L. Girardin, Carol Sánchez Santana, Courtney W. Mangus, Kelsie E. Mitchell, Amber R. Hughes, Becky Baltich Nelson, Bridget Gunn, Elizabeth M. Schoenfeld
- Teach-back method, Wikipedia
- README: Bridging Medical Jargon and Lay Understanding for Patient Education through Data-Centric NLP by Zonghai Yao, Nandyala Siddharth Kantu, Guanghao Wei, Hieu Tran, Zhangqi Duan, Sunjae Kwon, Zhichao Yang, README annotation team, Hong Yu
- From information to impact: Evolving patient education in modern care delivery, Walters Kluwer
- Decision Aids, Wikipedia
- Combating medical misinformation and rebuilding trust in the USA by Clara E Tandara, John C Linb, Fatima Cody Stanford
- Patient Trust in Physicians Matters—Understanding the Role of a Mobile Patient Education System and Patient-Physician Communication in Improving Patient Adherence Behavior: Field Study by Dezhi Wu, Paul Benjamin Lowry, Dongsong Zhang, Youyou Tao
- Approaches to Reach Trustworthy Patient Education: A Narrative Review by Xiafei Lyu, Jing Li, Sheyu Li